|
Before and After Weight Loss Success Photos. Age: 5. 0Pounds Lost: 5. Weight- Loss Tip: “I used to pick on fruit, yogurt, and crackers for lunch, but I’d snack all afternoon,” she says. Overview, Prevalence and Loss of Body Water, Assessing Fluid and Electrolyte Status. Goals for nutrition management. The primary goal in total parenteral nutrition (TPN) is to provide energy and nutrients in sufficient quantities to allow normal growth and development. Thereafter, daily weight is used in calculations. TPN can be started on the first day of life in infants who are not likely to achieve total enteral nutrition within the first week of life. Especially in infants who are ill, protein is required to decrease or prevent catabolism, and starting TPN on the first day is important. 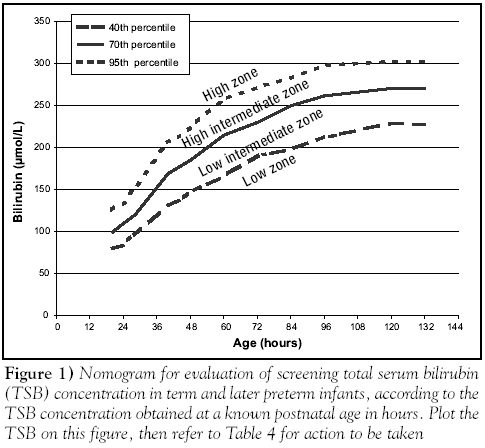
A standardized TPN solution (based on postnatal age) may be more convenient and cost- effective compared with individualized TPN. One kcal equals 4. 
J. Calculate the infant's daily fluid (water) requirement. Calculate the amount of energy required. Determine the specific amounts and sources of carbohydrates and lipids. 
In addition, determine the amounts of vitamins and trace elements to deliver. Determine the amount of protein to deliver based on the total number of calories to be provided. Remember that an infant needs an adequate number of nonprotein calories (6. J/g nitrogen) to have a positive nitrogen balance. 
Most practitioners start at 1. Various amino acid preparations are commercially available for use in the neonate (eg, Troph. Amine). Carbohydrate. IV dextrose provides most of the energy in TPN. The caloric content of aqueous dextrose is 1. J/g of glucose, which is equal to 1. J/1. 00m. L of D1. W. As a result of the high osmolarity of concentrated dextrose solutions, the maximum dextrose concentration that can be delivered safely through a peripheral vein is 1. With central venous access, a dextrose concentration up to 1. A glucose infusion rate expressed in milligrams of glucose/kg/min is the most appropriate way to express glucose administration because the rate accounts for the glucose concentration and the rate of infusion. Very small premature infants who weigh less than 1. For this reason, in infants who weigh less than 1kg, start at an infusion rate of 6mg/kg/min. In infants who weigh 1- 1. If the glucose infusion rate is excessive, hyperglycemia may develop. If blood glucose levels are greater than 1. L, glucosuria may occur, which may lead to osmotic diuresis. This can be controlled by either decreasing the glucose infusion rate or treating the infant with insulin. Persistent hyperglycemia may need a continuous infusion of insulin. Fat. At least 3% of the total energy should be supplied as essential fatty acids (EFA). This can be accomplished by providing a fat emulsion (eg, Intralipid, Liposyn), 0. Fat emulsions provide about 3. J/g. Parenteral fat emulsion is usually provided as a 2. Intralipid). Intralipid is a concentrated source of energy with a caloric density of 8. J/m. L (for 2. 0% Intralipid). Lipids play a primary role in supporting gluconeogenesis in parenterally fed preterm infants. 
The use of Intralipid (as well as prolonged TPN and use of central venous lines) is a risk factor for candidemia in neonates. Some evidence suggests that use of lipid infusions with omega- 3 fatty acids (eg, Omegaven) may reduce cholestasis, but further studies are currently required. Protein. Term infants need 1. Preterm VLBW infants need 3- 3. Usually, providing more than 4g/kg/day of protein is not advisable. Infants under stress or who have cholestasis are usually limited to 2. TPN- induced cholestasis may depend on the duration of TPN and the amount of amino acids infused. Maintain a nonprotein- to- protein calorie ratio of at least 2. 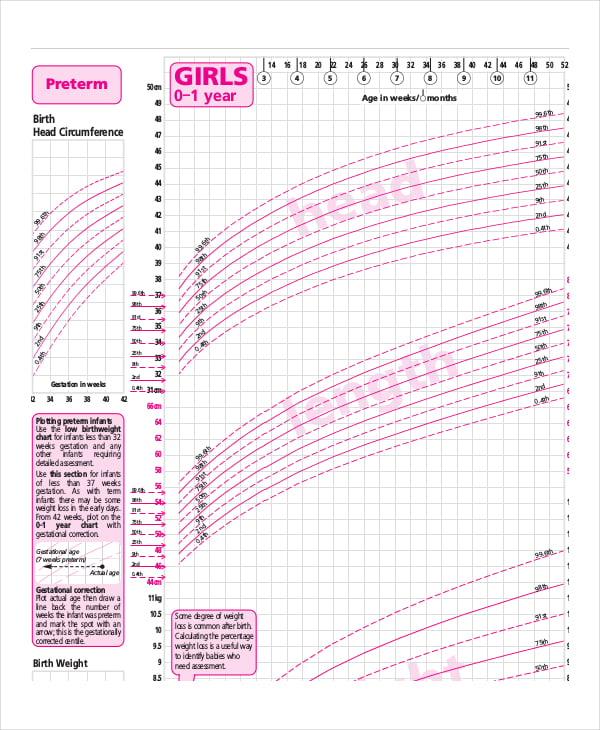
Order Focus T25! Back to Table of Contents. How To Get Your Best Focus T25 Results. Are you looking to get the best weight loss results possible with Focus T25? 
The current role of supplements, such as additional inositol and carnitine, is under investigation. Although a physiologic rationale for their use has been suggested, they have not yet been shown to be of benefit in large, randomized, controlled trials. Calcium and phosphorous need to be concurrently administered for proper accretion. Take care to ensure that solubility is not exceeded; if this happens, calcium and phosphorous may spontaneously precipitate. Supplemental magnesium should be added to TPN once protein has been added. Vitamins and trace elements. Vitamins A, D, E, and K are fat soluble. Vitamins B- 1, B- 2, B- 6, B- 1. C, biotin, niacin, pantothenate, and folic acid are water soluble. Vitamin supplementation should be started as soon as protein is added to TPN. The addition of a commercially available neonatal vitamin preparation provides appropriate quantities of all vitamins, except possibly vitamin A. Vitamin A supplementation in ELBW infants has been shown to reduce death and BPD. The trace elements zinc, copper, selenium, chromium, manganese, molybdenum, and iodine also should be added to TPN once protein is started. This can be easily accomplished by the addition of a commercially available solution containing trace elements.
Free weight loss tools and calculators - includes daily calorie needs, resting heart rate, calories burned, ideal body weight, body fat percentage and more.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
